
Overview
Quality Blue is an innovative health care quality improvement program that allows network providers opportunities to earn recognition and financial incentives by meeting performance indicators.
Louisiana Blue takes a leadership role in developing programs that reward providers for quality improvements that get better health results for patients while making health care more affordable.
Quality Blue recognizes providers who are working in collaboration with Louisiana Blue to transform health care systems and improve the way care is delivered to Louisiana Blue members - their patients - to help achieve better health outcomes.
Quality Blue encourages value-based (as opposed to volume-based) practice methods by equipping providers with a performance-based payment structure. Practices may be eligible to receive financial incentives for successfully achieving quality and total cost of care goals. Each attribute of Quality Blue was designed to successfully facilitate the necessary transformation to improve the health and lives of Louisianians.
Design
Quality Blue is a value-based payment program that encompasses all the value-based modules and is available to different providers and lines of business. It is designed as a modular approach to meet providers where they are, and support pathways to enhanced value-based payments over time on the path to Louisiana Blue's comprehensive reimbursement strategy.
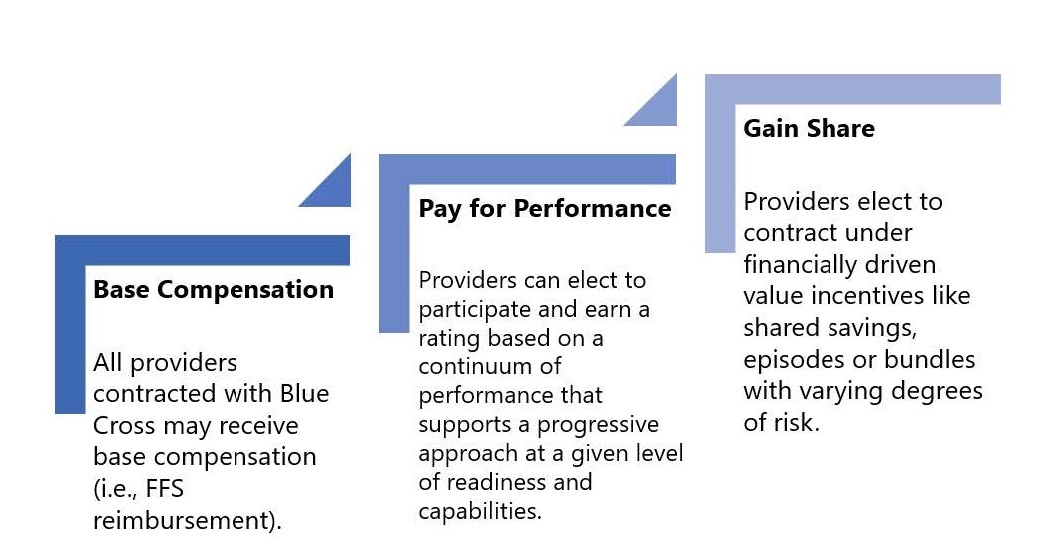
The Value Proposition
Louisiana Blue is a patient-centric population health and quality improvement program designed to transform our network from an episode-driven, provider care delivery model to a team-based care delivery model. Quality Blue addresses the needs of the populations we serve to improve Louisiana’s health outcomes.
For Practices:
For Members:
For Blue Cross:
Contact Us
To learn more about our QB program, please email our Provider Relations Department at provider.relations@bcbsla.com.